Revenue Cycle Management Company
A successful, reliable RCM service offering is key to the sustainability and growth of your business. Physicians, hospitals and ancillary healthcare service providers increasingly rely on their medical billing partners and Health IT vendors to be the subject matter experts on reimbursements and financial data, and to deliver measurable improvements in both top and bottom-line revenue streams.
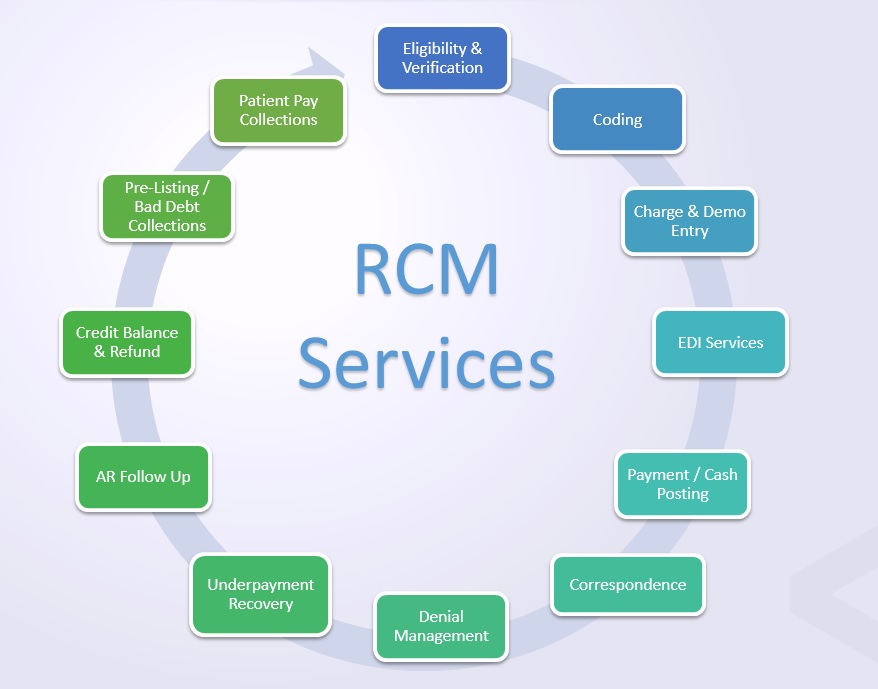
Hiring, training and maintaining that in-house knowledge and experience is costly and complex. Our revenue cycle management company can help you simplify your internal processes and reduce outlay without sacrificing quality or results. Our end-to-end revenue cycle outsourcing means that every stage of every claim is expertly managed, from detailed eligibility verifications to charge entry and payer submissions, adjudication and denial follow-ups, and comprehensive A/R management.
- Reduce days to bill: with clear eligibility and benefit details, and clean claims that are coded for maximum reimbursement
- Collect more, faster: with automated EDI services, detailed payment and cash posting, and some of the most diligent A/R teams in the industry working each claim to collect every dollar as if it were our own
- Streamline workflows: with proven processes for everything from denial management and underpayment recovery, to patient balance collections